Dr Amit Arora is a Consultant Physician and Geriatrician at University Hospital of North Staffordshire, Stoke on Trent and an Honorary Clinical Lecturer at Keele University.
 Many years ago I was subject to restricted mobility following an emergency appendicectomy. It took me a surprisingly long time to regain my strengths and abilities- I noted that despite the youth and the will, my muscles would not move and it took a while to recover back to normal!
Many years ago I was subject to restricted mobility following an emergency appendicectomy. It took me a surprisingly long time to regain my strengths and abilities- I noted that despite the youth and the will, my muscles would not move and it took a while to recover back to normal!
When I co-relate this to the frail older people that I see in hospitals, I can understand why someone who was able to function well before they came to hospital takes longer to regain their pre-admission functionality. Prolonged hospital stay, bed rest and attendant risks may lead to loss of muscle power, strength and abilities. This is something we surely need to avoid. It should help achieve a shorter length of stay, better outcomes for patients and better ability at discharge.
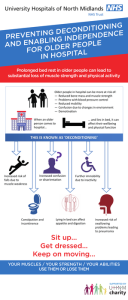
Older people in hospitals can have an increased risk of reduced bone mass and muscle strength, problems with blood pressure control, reduced mobility, increased dependence, confusion and demotivation. These problems can be attributed to deconditioning. This affects well-being as well as physical function and could result in falls, constipation, incontinence, depression, swallowing problems, pneumonia and leads to demotivation and deconditioning. Deconditioning occurs when older people in hospital lose their abilities to do daily activities over time, due to inactivity in hospital.
 Preventing deconditioning in hospitals requires an approach that includes physical therapy, maintenance of nutrition, medical management, and psychological support. Activity and independence should be promoted from the time of admission.
Preventing deconditioning in hospitals requires an approach that includes physical therapy, maintenance of nutrition, medical management, and psychological support. Activity and independence should be promoted from the time of admission.
But, are all health care staff and patients aware of the phenomenon of deconditioning? Are we doing enough to prevent deconditioning? Do we care?
Of course, we care!
We are caring professionals. But are we being over-caring to the point that we do everything for our patients, without attempting to encourage them to do what they can do themselves and supplementing it with our help?
 How can we help? Simple things first. We could ensure that glasses and hearing aids are readily available, ensure that patients are sat up in chairs, preferably in their own clothes and ensure that meals are consumed whilst sitting in chairs and not spoon fed in bed unless circumstances dictate so. We could encourage patients to wash and dress independently, walk to the toilet where possible, provide appropriate mobility aids earlier on and encourage patients to keep their arms and legs moving in bed or chair. Even moving arms, legs and sitting up in bed when examining chest offers a small degree of physiotherapy of its own kind. Removing catheters can help regain confidence. Removing restrictions on visiting hours and social interactions to encourage normalcy will also help to maintain functionality and regain independence.
How can we help? Simple things first. We could ensure that glasses and hearing aids are readily available, ensure that patients are sat up in chairs, preferably in their own clothes and ensure that meals are consumed whilst sitting in chairs and not spoon fed in bed unless circumstances dictate so. We could encourage patients to wash and dress independently, walk to the toilet where possible, provide appropriate mobility aids earlier on and encourage patients to keep their arms and legs moving in bed or chair. Even moving arms, legs and sitting up in bed when examining chest offers a small degree of physiotherapy of its own kind. Removing catheters can help regain confidence. Removing restrictions on visiting hours and social interactions to encourage normalcy will also help to maintain functionality and regain independence.
Patients need to be supported and encouraged to get moving as quickly as possible, within their current limits. As leaders it is our role to encourage our staff to in-turn encourage our patients to do what they can.
That would mean, ‘we really care’! Staff and families have an important role to play in preventing deconditioning. Education of patients, relatives, carers and staff about the dangers of deconditioning is vital, since bed rest continues to be expected during a hospital stay, despite the considerable evidence showing potential adverse effects from inactivity. Of course there are times and conditions when bed rest would be advisable; but more often than not, this is not the case in the strictest terms.
 Reconditioning can take twice as long as deconditioning; if it has taken one month to get to this low level of function, it may take two months of hard work to return to their original level. It is often said that for every 10 days of bed rest in hospital, the equivalent of 10 years of muscle ageing occurs, in people over 80 years old.
Reconditioning can take twice as long as deconditioning; if it has taken one month to get to this low level of function, it may take two months of hard work to return to their original level. It is often said that for every 10 days of bed rest in hospital, the equivalent of 10 years of muscle ageing occurs, in people over 80 years old.
If we want the best outcomes for our patients, it is necessary to design effective programs for reconditioning. We need to get our patients up as quickly as possible, while being careful not to overload them. In terms of frequency of sessions, it is more beneficial for patients to do several smaller sessions rather than one long session.
We need a strategy to combat deconditioning which includes a model of care appropriate to the growing population of elderly people, the creation of an “elder-friendly” hospital environment and an exercise program. This will have to be thought out clearly and may cost more in the short term, but with major long term societal health gains.
This Older Peoples’ day, we have launched a deconditioning awareness campaign for staff and patients across some of our hospitals. There are banners, posters, screensavers, information leaflets, exercise programs and live demonstrations to raise awareness. I am more than happy to provide additional information and share material to make this a success.
Get up, Get Dressed, Keep moving….
Your muscles, Your strengths, Your abilities: use them or lose them.
Dr Amit Arora and colleagues at UHNM wish to acknowledge the work from various authors and contributors who this campaign has received inspiration from and these include various articles and images on the internet and in particular but not exclusively the work of Gillis A et al, Carol Lewis, colleagues from ECIST, AFN, BGS, NHS England and Philip Holmes et al from Salford Royal NHS Foundation trust.
The material contained here is available freely for use for benefit of patients.

Thank you for such a thoroughly sensible article — and for advocating the removal of restrictions on visiting hours so that families can assist with this. As the daughter of a 92 year old with dementia I consider that keeping her moving is one of the more useful things I do. I’m also involved with John’s Campaign for carers access. Not quite sure how your hospital is progressing with this, do you know? Thanks again for your article
Pingback: Contra la “discapacidad iatrogénica nosocomial”: levántate, vístete, muévete | hablandodegeriatria
This is music to my ears! As a physiotherapist I have been trying to promote physical activity amongst patients and influence managers to support I’ve in doing so, not easy with conflicting agendas. Where can I get hold of the resources shown? I’m start work in a new frailty unit in Harrogate more information would be massively useful for me, my patients and my colleagues!
Pingback: Sit up, Get Dressed, Keep Moving: Deconditioning Syndrome Awareness and Prevention Campaign: why is everyone talking about it? | British Geriatrics Society